The act of swallowing (degluttition) is an intricate action involving the integration of a complex series of sensory and motor responses. The act of swallowing must occur in a sequential and coordinated fashion in order to propel the food bolus into the esophagus and stomach without penetration into the larynx (voice box) and airway (lungs). This process is so complex that it is remarkable that most of us don’t have to think about swallowing at all. It is this complexity that results in the extensive number of impairments that can occur with the swallowing mechanism.
The swallowing mechanism can be divided into 4 phases:
- Oral preparatory phase
- Oral Phase
- Pharyngeal Phase
- Esophageal Phase.
Oral Phase
In the oral phase numerous difficulties can arise. Problems of weakness of the lips, tongue and cheeks due to stroke, or degenerative neurological conditions can cause problems keeping food in the mouth. Such neurologic disorders prevent an individual from organizing the food into a well-formed bolus and moving it posteriorly in the mouth. If there is specific unilateral cheek (buccal) weakness, food can enter a pocket in one cheek making eating unsafe. Problems with xerostomia (dry mouth) such as after radiation therapy can result in difficulty breaking down solids and difficulty swallowing them smoothly through the hypopharynx. If someone has had oral cancer and has actually had part of the lips, tongue, cheek or palate removed, similar problems can occur with containing, masticating and transporting food through the mouth.
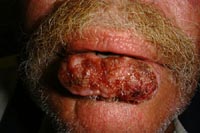 The image below is a patient with an advanced squamous cell carcinoma of the lower lip who lost 25 pounds because of impairment of the oral phase of swallowing.
The image below is a patient with an advanced squamous cell carcinoma of the lower lip who lost 25 pounds because of impairment of the oral phase of swallowing.
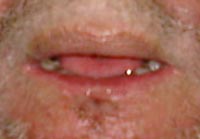 Successful resection of the cancer with reconstruction and aggressive therapy with a speech language pathologist resulted in complete resolution of the swallowing disorder. See the postoperative image below.
Successful resection of the cancer with reconstruction and aggressive therapy with a speech language pathologist resulted in complete resolution of the swallowing disorder. See the postoperative image below.
Pharyngeal Phase
The most common problems that occur in the pharyngeal phase can be categorized into problems of timing and weakness. Problems with timing usually occur in patients with neurological deficits. In such persons, the swallow reflex does not trigger effectively enough for the larynx to be protected beneath the epiglottis. This may result in penetration or aspiration of food or liquids. When the food passes through the vocal folds (aspiration) the patient may cough in an attempt to expel the dangerous food particles from the airway. In certain patients, however, the cough response may be diminished and aspiration may occur without any warning at all. This is referred to as “silent aspiration”. Silent aspiration is very dangerous and may result in aspiration pneumonia or even death. Therefore, the trained swallowing specialist does not rely on the presence of coughing alone when assessing the patient’s swallowing function and will often request further diagnostic testing, such as a modified barium swallow or endoscopic evaluation of swallowing.
The cricopharyngeus muscle, also referred to as the upper esophageal sphincter (UES), may occassionally malfunction. It may be hypertonic, fail to relax, or work in a discoordinated fashion. UES dysfunction can cause dysphagia, weight loss, a sensation of food getting stuck in the throat, and aspiration. Appropriate relaxation of the UES is essential to the normal swallowing mechanism. Abnormalities can be evaluated by UES manometry. Treatment may be chemical (Botox) or surgical. Significant abnormality of the UES may result in an upper esophageal diverticulum (See section on Zenker’s Diverticulum).
Click on the image at the top of the page to view a modified barium swallow of an individual with cricopharyngeal dysfunction. The resting tone of this person’s UES was extremely elevated and failed to relax appropriately during degluttition. Notice the prominent, hypertonic UES on the examination. Several repeat swallows are necessary to pass the residual barium. The patient’s cricopharyngeus was injected with 10 units of botox bilaterally under manometric guidance. The dysphagia completely resolved within 48 hours after the injection.
Problems of weakness, usually the result of neurological injury, can also occur after cancer of the throat with subsequent surgery. Because the muscles that push the food through the pharynx are weak, there is residue of food in the pharynx after the swallow. The residual food particles can then enter into the airway and cause pneumonia. It is not uncommon for neurologically impaired patients to be unaware of residue in the throat. Therefore, relying on the patient’s report of swallowing difficulties is not an accurate method of determining swallowing risk or safety. If the muscles of the pharynx are too weak to propel food safely into the esophagus, aggressive swallowing therapy with the application of various swallowing techniques may improve pharyngeal strength and limit aspiration. In certain individuals surgically weakening the upper esophageal sphincter (cricopharyngeal myotomy) to ease transport through a weakened pharynx may be beneficial. This can be done chemically with the use of Botox or surgically through an open procedure (more invasive but also more permanent).
Esophageal Phase
Finally, patients can have difficulties in the esophageal phase of the swallow due to problems with esophageal peristalsis (the wave-like squeezing action of the muscles of the esophagus that is necessary to propel food down the swallowing pipe), tumor, or stricture. A tumor in the esophagus or a stricture from reflux or chemical injury can cause a mechanical obstruction with difficulty passing food. Surgically removing the tumor or dilation of the stricture will relieve the dysphagia (difficulty swallowing) in most cases.
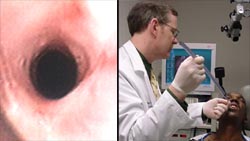 The following image is a composite of an individual with epidermolysis bullosa and an upper esophageal stricture. The patient underwent transnasal esophagoscopy (TNE) with dilation of the stricture in the office without any sedation. He had minimal discomfort during the 5 minute procedure, his dysphagia (swallowing difficulty) was immediately resolved, and he went home the same day.
The following image is a composite of an individual with epidermolysis bullosa and an upper esophageal stricture. The patient underwent transnasal esophagoscopy (TNE) with dilation of the stricture in the office without any sedation. He had minimal discomfort during the 5 minute procedure, his dysphagia (swallowing difficulty) was immediately resolved, and he went home the same day.
Normal esophageal peristalsis is essential in passage of the food bolus through the esophagus and into the stomach. Any disorder in esophageal peristalsis such as scleroderma, nutcracker esophagus (NE), non-specific esophageal motility disorder (NEMD) or diffuse esophageal spasm (DES) can cause problems with the esophageal phase of the swallow. Identifying the inciting cause is essential in formulating a successful treatment regimen.
Various patients can have multiple deficits. For example, a stroke patient with a poorly coordinated pharyngeal phase of swallowing can have an esophageal motility disorder that was pre-existing. An edentulous (no teeth) patient with a pharyngeal tumor removed who also received radiation therapy may have problems with both the oral and pharyngeal phase. Our approach to the person with a swallowing disorder at the UC Davis Center for Voice and Swallowing is to correctly identify each underlying disorder so that an aggressive treatment strategy may be instituted.
We employ a vast array of non-invasive diagnostics including pharyngeal and esophageal manometry, endoscopic evaluation of swallowing, esophagoscopy, and cinevideofluroscopy (modified barium swallow) to achieve our goal. We have assembled experts in the fields of speech language pathology, otolaryngology, gastroenterology, neurology, and pulmonology to provide a comprehensive multidisciplinary approach to the patient with a swallowing disorder. Various surgical treatments such as laryngohyoid suspension, great auricular to superior laryngeal nerve neurroraphy, and medialization laryngoplasty are utilized in select patients.
