Treatment for reflux can be divided into 3 separate categories or “phases.” These phases range from behavioral modifications, such as the avoidance of caffeine and alcohol to surgical intervention. The three phases are detailed below.
Phase I therapy – Behavioral Modification, Gum, and Antacids
Elevate the head of bed 6 to 8 inches. This will keep gravity on your side and help prevent stomach contents from refluxing back up the esophagus when you lie down. Propping your head up on pillows will not achieve this goal and may actually make the problem worse. Buying a bed wedge is the easiest way to accomplish this goal. A wedge support pillow may cost from $20 to $50. These can be found on http://www.amazon.com.
If you are overweight, lose weight.
Avoid tobacco and foods high in fat, spices, acid, alcohol, and caffeine. This includes cigars, cigarettes, coffee, soda, caffeinated tea, citrus juice, fried food, beer and wine. One cup of decaffeinated coffee can stay in your system for 16 hours.
Scand J Gastroenterol Suppl. 1999;230:35-9.
Coffee and gastrointestinal function: facts and fiction. A review.
Boekema PJ, Samsom M, van Berge Henegouwen GP, Smout AJ.
Dept. of Gastroenterology, University Hospital Utrecht, The Netherlands.
BACKGROUND: Effects of coffee on the gastrointestinal system have been suggested by patients and the lay press, while doctors tend to discourage its consumption in some diseases. METHODS: The literature on the effects of coffee and caffeine on the gastrointestinal system is reviewed with emphasis on gastrointestinal function. RESULTS: Although often mentioned as a cause of dyspeptic symptoms, no association between coffee and dyspepsia is found. Heartburn is the most frequently reported symptom after coffee drinking. It is demonstrated that coffee promotes gastro-oesophageal reflux. Coffee stimulates gastrin release and gastric acid secretion, but studies on the effect on lower oesophageal sphincter pressure yield conflicting results. Coffee also prolongs the adaptive relaxation of the proximal stomach, suggesting that it might slow gastric emptying. However, other studies indicate that coffee does not affect gastric emptying or small bowel transit. Coffee induces cholecystokinin release and gallbladder contraction, which may explain why patients with symptomatic gallstones often avoid drinking coffee. Coffee increases rectosigmoid motor activity within 4 min after ingestion in some people. Its effects on the colon are found to be comparable to those of a 1000 kCal meal. Since coffee contains no calories, and its effects on the gastrointestinal tract cannot be ascribed to its volume load, acidity or osmolality, it must have pharmacological effects. Caffeine cannot solely account for these gastrointestinal effects. CONCLUSIONS: Coffee promotes gastro-oesophageal reflux, but is not associated with dyspepsia. Coffee stimulates gallbladder contraction and colonic motor activity.
Aliment Pharmacol Ther. 1997 Jun;11(3):483-6.
The effect of decaffeination of coffee on gastro-oesophageal reflux in patients with reflux disease.
Pehl C, Pfeiffer A, Wendl B, Kaess H.
Department of Gastroenterology, Hospital Bogenhausen, Munich, Germany.
BACKGROUND: Patients with reflux disease often complain of heartburn after ingestion of coffee. Induction of gastro-oesophageal reflux has been demonstrated by pH-metry following the intake of coffee in healthy volunteers. The reflux was reduced when the coffee had undergone a decaffeination process. The aim of this study was to investigate the effect of decaffeination of coffee on reflux in patients with reflux disease. METHODS: Seventeen reflux patients underwent two osesophageal 3-h pH measurements. The patients received, in a double-blind study design in a randomized order, 300 mL of either regular or decaffeinated coffee together with a standardized breakfast. The fraction time oesophageal pH < 4 was calculated during the three postprandial hours. RESULTS: For regular coffee the fraction time was calculated to a median of 17.9% with a range of 0.7-56.6%. The fraction time was significantly reduced to 3.1% (0-49.9%) after ingestion of decaffeinated coffee. CONCLUSION: The amount of gastro-oesophageal reflux induced by the intake of regular coffee in patients with reflux disease can be reduce by the decaffeination of coffee.
Gastroenterology. 1995 Jan;108(1):125-31.
Relationships between the acidity and osmolality of popular beverages and reported postprandial heartburn.
Feldman M, Barnett C.
University of Texas Southwestern Medical School at Dallas.
BACKGROUND/AIMS: Although many beverages produce heartburn, the relationship between the acidity and osmolality of beverages and heartburn is unclear. The aim of this study was to relate the acidity and osmolality of beverages with their ability to cause heartburn. METHODS: We measured pH, total titratable acidity, and osmolality of 38 beverages in vitro and then correlated acidity and osmolality with the amount of heartburn reported by questionnaire in 394 people with heartburn. RESULTS: Among 17 citrus drinks and juices, titratable acidity correlated with reported heartburn scores (r = 0.65; P = 0.004). Soft drinks had the lowest pH readings of any beverages studied, and decreasing pH among soft drinks was correlated with reported heartburn scores (r = 0.82; P < 0.001). Alcoholic beverages (wines and beer), coffee, and (to a lesser extent) tea were associated with significant amounts of reported heartburn when compared with water. Milk was also associated with a modest amount of reported heartburn that was related to its fat content. Osmolality of beverages was unrelated to reported heartburn. CONCLUSIONS: High titratable acidity of citrus drinks and juices and low pH of soft drinks are associated with more reported heartburn. Our findings provide a foundation for dietary advice in patients with heartburn and reflux esophagitis.
Do not lie down immediately after eating. A stomach full of food is more likely to regurgitate up the esophagus. This means that you should try and not have anything to eat or drink for 3 hours before bed.
Avoid drugs that can promote reflux. These include calcium channel blokers, sedatives, alcohol, nitrates.
Take antacids as needed. Antacids such as Maalox and Tums may be taken 30 minutes after meals, before bedtime, and as needed. They are successful for the treatment of mild reflux disease. They act by neutralizing the acid produced by the stomach.
Alginate-based reflux suppressants can prevent the regurgitation of gastric contents. Gaviscon Advance is a product available in Europe only (www.gaviscon.co.uk). It contains 1000mg of sodium alginate/10ml. Alginate is a natural product deived from seaweed. The alginate reacts with the acid in the stomach to produce a “raft” on the stomach that acts as a physical barrier to reflux. It is the only non-surgical treatment that can physically prevent reflux disease. Alginates work rapidly, are long lasting, inexpensive, and have no known side-effects. Gaviscon in the USA is made by a different company. Although all gaviscon products in the US have alginate in them, it is in a much lower dose and is considered an inactive ingredient. It does not appear to be as effective as the UK product.
Aliment Pharmacol Ther. 2005 Jan 1;21(1):29-34
An evaluation of the antireflux properties of sodium alginate by means of combined multichannel intraluminal impedance and pH-metry.
Zentilin P, Dulbecco P, Savarino E, Parodi A, Iiritano E, Bilardi C, Reglioni S, Vigneri S, Savarino V.
Dipartimento di Medicina Interna e Specialita Mediche, Universita di Genoa, Genoa, Italy.
BACKGROUND: Alginate-based preparations act as mechanical antireflux barrier, which can reduce both acid and non-acid reflux events and limit the proximal migration of oesophageal refluxate. AIM: To evaluate all the above features with a novel technique, multichannel electrical impedance and pH-metry. METHODS: Ten reflux patients underwent stationary impedancemetry and pH-metry after eating a refluxogenic meal. They were studied 1 h in basal conditions and 1 h after taking 10 mL of Gaviscon Advance. In both sessions, measurements were obtained in right lateral and supine decubitus. RESULTS: Alginate preparation was able to decrease significantly (P < 0.05) the number of acid reflux events and the percentage time pH < 4.0 compared with baseline. There was no effect of the drug on non-acid refluxes. Gaviscon Advance was also significantly effective (P < 0.05) in reducing the height of proximal migration of reflux events compared with baseline in both decubitus positions. CONCLUSIONS: Our findings explain how Gaviscon Advance controls acid reflux episodes, limits the proximal migration of refluxed material and thereby decreases symptoms in clinical practic
Chew Gum. Gum, especially bicarbonate gum, has been shown to increase salivary bicarbonate and prevent reflux. Bicarbonate gum (baking soda gum) can usually be found in the tooth pasteisle of the pharmacy (it is also good for the teeth).
Ann Otol Rhinol Laryngol. 2001 Dec;110(12):1117-9.
Effects of gum chewing on pharyngeal and esophageal pH.
Smoak BR, Koufman JA.
Center for Voice Disorders of Wake Forest University, Winston-Salem, North Carolina 27157-1034, USA.
We investigated the effects of gum chewing on pharyngeal and esophageal pH levels in patients with laryngopharyngeal reflux (LPR) who were undergoing reflux testing. Forty consecutive, unselected, adult patients who were undergoing ambulatory double-probe (simultaneous pharyngeal and esophageal) pH monitoring for diagnosis of LPR were asked to chew 2 sticks of gum 4 times during their pH studies. Twenty subjects chewed regular sugarless gum, and 20 subjects chewed a sugarless gum containing bicarbonate. The subjects recorded the beginning and end of each gum-chewing period. The mean pH values for the gum-chewing intervals and for comparable pre-gum-chewing intervals were analyzed statistically for both the pharyngeal and esophageal probe data. The regular gum group and the bicarbonate gum group were analyzed separately. In addition, the gum-chewing pH data were compared to controls, ie, normal postcibal buffering effects. The data show that gum chewing consistently increases esophageal and pharyngeal pH, and that bicarbonate gum causes greater increases than regular gum. For patients with LPR, gum chewing appears to be a useful adjunctive antireflux therapy.
Phase II therapy – Pharmacotherapy
H2 Antagonists. H2 blockers, such as Pepcid or Zantac may be instituted. These medications are now available over-the-counter without a prescription. They may be taken 2 to 3 times a day. Treatment may be continued for 6 to 8 weeks. After this initial treatment period, a trial of tapering these medications should be attempted. These drugs block histamine H2-receptors and reduce acid secretion. they can reduce acid output by about 50%. They can relieve symptoms in persons with mild reflux disease.
Proton Pump Inhibitors (PPIs). PPIs such as Prilosec, Prevacid, Nexium, Aciphex, and Protonix are an entirely different class of medication than the H2 blockers. They are generally more effective at preventing symptoms of GERD and LPR and healing esophagitis and chronic laryngitis. Prilosec (omeprazole) is now available without a prescription. These medications work by inhibiting the gastric parietal cell proton pump. They can reduce acid production by 80-90% if taken twice a day. Treatment is usually begun once daily for non complicated GERD and twice daily for LPR. Patients with LPR require higher doses of medication in order to achieve complete acid suppression and heal the delicate laryngeal tissue. Tissue injury in LPR may take 6 months to reverse once adequate therapy has been initiated. Severe, complicated cases may require the addition of an H2 blocker or even a third daily dose. Patients should not stop these medications abruptly because a rebound hypersecretion of gastric acid may occur. These drugs should be stopped gradually over a period of several weeks. It is important to note that these medicines do not prevent the regurgitation of stomah contents. they simply remove acid from the equation. Food can still come up and cause throat irritation, throat clearing, cough, and hoarseness.
Other medications such as prokinetic agents (Metoclopramide and Cisapride) and sucralafate are available. Severe, complicated cases may require medications from multiple classes.
Phase III therapy – Surgery
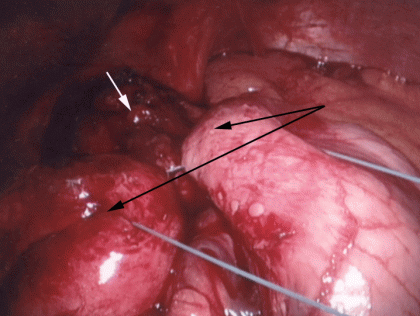
Surgical therapy generally consists of what is called a Nissen fundoplication. This procedure tightens the lower esophageal sphincter by wrapping the upper part of the stomach around the lower part of the esophagus. The procedure may be performed open with external incisions on the abdomen, however, newer endoscopic technology is now available which no longer require large external incisions. The endoscopic approach causes much less discomfort as well as a shorter hospital stay. As many as 90 percent of patients undergoing the laparoscopic Nissen fundoplication are symptom free after surgery. The surgery is performed by a general surgeon. Indications for surgery in patients with GERD and LPR include failure of medical therapy, the long time need for high dose medical therapy, severe erosive esophagitis, laryngitis, subglottic stenosis, or ulceration, aspiration of refluxed stomach contents, and Barrett’s esophagus. Comlications of the procedure include dysphagia and bloating. Both are usually transient and resolve completely. the image below shows a view of a laparoscopic Nissen Fundoplication. The black arrows point to the fundus wrapped around the esophagus (white arrow) creating a valve for the prevention of reflux.
J Am Coll Surg. 2004 Jul;199(1):23-30.
Fundoplication for laryngopharyngeal reflux disease.
Westcott CJ, Hopkins MB, Bach K, Postma GN, Belafsky PC, Koufman JA.
Department of General Surgery, Wake Forest University School of Medicine, Winston-Salem, NC 27157, USA.
BACKGROUND: Laryngopharyngeal reflux (LPR) disease arises from the effects of refluxed gastric contents on the proximal aerodigestive tract. LPR patients are often lumped into the category of “atypical” reflux. LPR symptoms are hoarseness, globus, cough, and pharyngitis. Severe disease is associated with subglottic stenosis and laryngeal cancer. Treatment includes lifestyle modifications and medications. The role of fundoplication for LPR has yet to be defined. STUDY DESIGN: Forty-one patients underwent fundoplication for LPR. They were prospectively followed with three outcomes measures: The Reflux Symptom Index, a laryngoscopic grading scale (Reflux Finding Score), and a reflux-based specific quality-of-life scale. RESULTS: Average early followup was at 4 months and late followup was at 14 months. The Reflux Symptom Index improved by 5.4 early (p < 0.05) and 6.5 late (p < 0.05). Improvement between early and late periods approached significance (p < 0.09). Reflux Finding Score improved 3.8 (p < 0.05) early and 4.4 (p < 0.05) late. The Quality of Life Index improved 0.6 early and 2.3 (p < 0.05) late. By Reflux Symptom Index criteria, 26 patients were improved early versus 35 late (p < 0.05). Factors associated with poor outcomes were structural laryngeal changes in five patients (p < 0.05) and no response to proton pump inhibitors in six patients (p < 0.05). CONCLUSIONS: Fundoplication augments treatment of LPR. Improvement of symptoms continues past the first 4 months. Laryngoscopy is critical in patient selection because selected findings are associated with outcomes, diagnosis, and management.
Alternative minimally invasive procedures. Alternative procedures such as endoscopic suturing and radiofrequency ablation of the lower esophageal sphincter are available. There efficacy in the long term treatment of GERD and LPR is uncertain.
Special Considerations for Patients with Esophageal Dysmotility
If you are reading this section you may have been diagnosed with esophageal dysmotility. Esophageal dysmotility is when the ability of the esophagus to contract and transport food and saliva from the mouth to the stomach has been diminished. Causes of ineffective esophageal motility (IEM) include:
- Advancing age (presbyesophagus)
- The prolonged effect of acid reflux over time
- Diabetes
- Achalasia
- Chagas Disease
- Scleroderma
- Polymyositis
- Parkinson’s Disease
- Amyotrophic Lateral Sclerosis (ALS)
- Thyroid disease
- Certain drugs
Symptoms of esophageal dysmotility can mimic gastroesophageal and laryngopharyngeal reflux disease. These symptoms include heartburn, dysphagia, regurgitation, cough, throat clearing, globus, and hoarseness. It is very import to diagnose ineffective esophageal motility as a cause of these symptoms because these symptoms do not improve with traditional anti-reflux medication and can get much worse with surgical anti-reflux therapy. Antacids and proton pump inhibitors do not usually help. They may be prescribed, however, to prevent further esophageal damage. If you have ineffective esophageal motility you must realize that YOU ARE NOT NORMAL. You can NOT eat a regular meal like a normal individual. If you eat a large meal at one sitting, a significant proportion of the food may sit in your esophagus for a very long time. The food can regurgitate out of the esophagus and cause cough, heartburn, symptoms in the throat, and even be aspirated into the lungs. Eating a large meal for someone with esophageal dysmotility can be devastating. Behavioral modifications are essential and include:
- Eat small, frequent meals. You MUST learn to eat like a goat. Snack and graze throughout the day. Avoid large and even medium sized meals.
- Never lay down after eating. The food sitting in your esophagus can regurgitate and end up in your lungs. Give yourself 3 hours after eating before laying down.
- Consume liquid alginate products after meals. If you live in the US and know anyone in the UK try getting them to send you Alginate Advance. The alginate can form a raft and help keep the esophageal contents down. If you can not get Alginate Advance from the UK take liquid Gaviscon 30cc after meals.
- Be very careful about taking pills. Pills can spend a very long time in your esophagus and cause a lot of damage. Try getting liquid formulations of your medicines if possible.
- Eat sitting bolt upright only. Gravity can help empty the esophagus.
- Avoid acidic foods. The acidic foods can pool in your esopphagus and contribute to the sensation of heartburn.
- Exercise and Lose weight. Exercising after meals may exacerbate your symptoms and should be avoided. Eat after exercising.
- Your doctor may prescribe prokinetic medication. These medications improve the ability of the esophagus to contract. They have limited efficacy and poor side-effect profiles, however. Their routine use is avoided.
